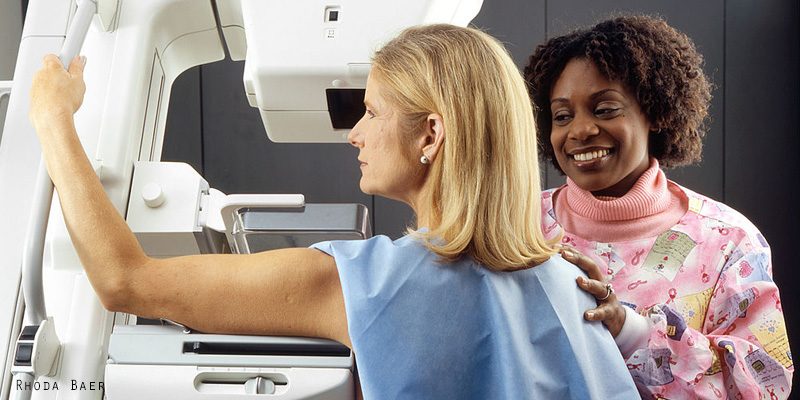
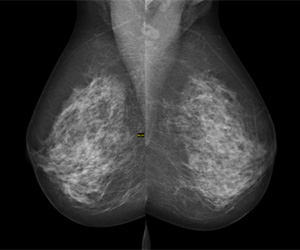
Dr. Manisha Bahl is a breast imaging radiologist and director of the Breast Imaging Fellowship Programme at Massachusetts General Hospital / Harvard Medical School in Boston. She is working with researchers from MIT’s Computer Science and Artificial Intelligence Laboratory (CSAIL) to improve breast cancer detection. Mammograms often result in false positive results that can lead to unnecessary biopsies and surgeries, so Manisha and her colleagues believe the answer is to turn to artificial intelligence (AI).

“…Use of our model has the potential to decrease unnecessary surgery by nearly one-third in women with high-risk breast lesions…”
Fascinated by science and the human body
I attended Stanford and UC-San Francisco for college and medical school, respectively, and graduated from the Harvard School of Public Health with an MPH in Health Policy and Management. I completed a radiology residency and breast imaging fellowship at Duke University Medical Centre. After a long road of training, I was excited to join the faculty at Massachusetts General Hospital / Harvard Medical School in July 2016.
I have always been fascinated by science and the human body and so decided to pursue medicine at a young age. As a doctor, I enjoy working with and helping patients and also solving challenging and complex problems. I was drawn to breast imaging early in my radiology training because of the opportunities to work directly with patients and collaborate with the multidisciplinary breast cancer care team.
A multi-faceted role
My day-to-day work includes clinical care, teaching, and research. My clinical work involves interpreting breast imaging exams, consulting with patients, and performing biopsies. I love working in the academic environment, where I can teach medical students, residents, and fellows, and also advance our field through research.
Interpreting mammograms
My colleagues and I perform image-guided breast biopsies every day. Image-guided biopsies that we perform based on suspicious findings on mammography can yield one of three pathology results: cancer, high-risk, or benign.
Most high-risk breast lesions are noncancerous, but surgical excision is typically recommended because some high-risk lesions can be upgraded to cancer at surgery.
Currently, there are no features (imaging or otherwise) that reliably allow us to distinguish between high-risk lesions that warrant surgery from those that can be safely followed, which has led to unnecessary surgery of high-risk lesions that are not associated with cancer.
New model to avoid unnecessary surgery
We decided to apply machine learning algorithms to help us with this challenging clinical scenario: to distinguish between high-risk lesions that warrant surgery from those that can be safely followed.
Machine learning allows us to incorporate the full spectrum of diverse and complex data that we have available, such as patient risk factors and imaging features, in order to predict which high-risk lesions are likely to be upgraded to cancer and, ultimately, to help our patients make more informed decisions about surgery versus surveillance.
Artificial Intelligence application improves clinical practice
Our study provides proof of concept that artificial intelligence can be used to predict the risk of upgrade of high-risk breast lesions to cancer. Use of our model has the potential to decrease unnecessary surgery by nearly one-third in women with high-risk breast lesions, sparing patients the costs and complications associated with surgery.
There is increasing interest in the application of artificial intelligence / machine learning to radiology in order to improve clinical practice, and it has the potential to dramatically affect the practice of radiology.
Artificial intelligence is being applied to many other areas in radiology – for example, to detect haemorrhage in the brain, to differentiate between cancerous and noncancerous nodules in the lungs, and to segment tumours in the liver.
Working in cross functional research teams achieves positive outcomes
It has been such a privilege to collaborate with researchers from MIT [Massachusetts Institute of Technology]. Our teams at Massachusetts General Hospital and MIT bring different skillsets, experiences, and perspectives to the table but are united with a common goal – to improve patient care.
Next steps with artificial intelligence
As mentioned above, our projects are currently focused on improving breast cancer detection with mammography. Moving forward, we are actively working to incorporate the high-risk breast lesion risk prediction tool into our daily clinical practice and hope to use it to guide clinical decision making very soon. The next step of this work is to incorporate the actual mammographic images and histopathology slides into our model.
We are also working on multiple other projects with researchers from MIT, all of which are related to artificial intelligence and how it can be used to improve breast cancer care.
http://www.massgeneral.org/doctors/doctor.aspx?id=19887
https://twitter.com/MassGeneralNews
https://www.facebook.com/massgeneral
Mammogram image credit (main image): By Rhoda Baer (Photographer) [Public domain or Public domain], via Wikimedia Commons
Digital mammography image credit: © Nevit Dilmen [CC BY-SA 3.0 (https://creativecommons.org/licenses/by-sa/3.0) or GFDL (http://www.gnu.org/copyleft/fdl.html)], via Wikimedia Commons